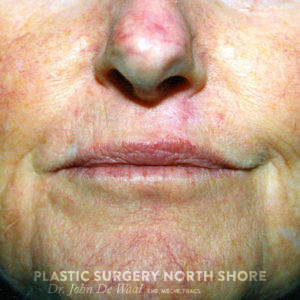
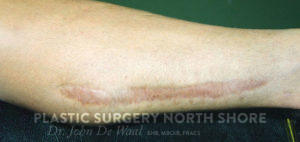
Scars
Whenever a wound is made, whether accidentally, intentionally or from a surgical procedure a scar forms because scar tissue is the way the body heals wounds. Generally, scars naturally improve with time as they mature. Scar tissue itself however, while becoming more organised and less conspicuous never actually goes away. If an ugly, irritable or troublesome scar is formed then it cannot be ‘removed’.
An attempt however can be made to improve its features:
- position
- contour
- width
- irritability
- related contractures – etc to render them less visible or problematic
There are generally 3 types of scars recognised:
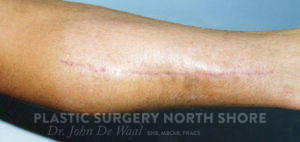
- STANDARD ‘normal’ scars – normal scars get redder, harder, lumpier during the scar healing phase (approx 6wks) and soften and fade in the scar maturation phase (approx 6mths)
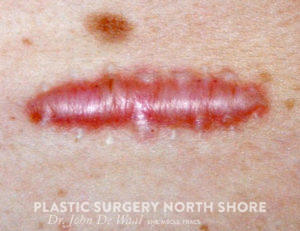
- HYPERTROPHIC scars – these are ‘overgrown’ or thickened scars. They tend to heal and mature like standard scars but often some irritating process (tension, infection, abrasion etc) has caused an excessive burden of scar to be laid down within the injured tissue and so they ‘heal’ over an extended period of time (6mths of the scar being red and thick before starting to mature over 12-24mths). There is a high risk of these type of scars on the shoulders and on the upper chest esp in women partly related to the tension produced by the weight of the breasts
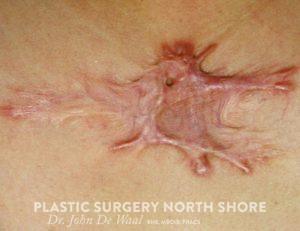
- KELOID – These scars ‘grow’ and lay down collagen outside the site of injury. A small scar then can literally grow into a large scar without any further injury. They are are distinctly abnormal type of scar and their unique character can be identified even by their appearance under the microscope. They are more common in ethnicities with darker pigment and so probably have a genetic component. For unknown reasons they grow and mature unpredictably and treatment strategies are frequently disappointing. Some consider these a type of scars a tumour and are sometimes even treated as such with radiotherapy
Non surgical treatment varies according to scar type
STANDARD SCARS
Scar treatments work best in the ‘collagen healing phase’ of scar healing (i.e – approx the first 6wks)
Remember all normal scars improve visually with time simply due to scar maturation and so before and after photos seen in advertising for scar gels and creams are misleading as all normal scars will show a significant improvement with time alone.
Occlusive dressings (simple tape, hydrocolloid dressings) and Silicone gel statistically reduces scar lumpiness and redness and aid the rate of scar maturation probably my keeping the scars moisteurised and providing protection from external irritation.
Wound support – from taping, deep sutures etc reduces scar width
HYPERTROPHIC SCARS
Because the collagen deposition phase is longer than in regular scars the treatment must be prolonged also.
As a general rule; as long as the scar is red, it is still immature and therefore can still get worse but is also amenable to non-surgical manipulation.
Hypertrophic scars tend to respond well to surgical revision if one can remove any contributing factors
- scar abrasion – a protective cover eg silicone gel can be effective
- remove foreign debri
- decrease tension on scar – eg. wear a supportive bra if the scar is on the upper chest in a woman
Steroid injections into the scar can often bring about softening and flattening of the scars and also reduce any associated itching. Often, however, the injections will need to be repeated several times.
KELOID SCARS
Treatment is highly unpredictable and none is guaranteed. In fact simple surgical excision has a greater than 20% chance of making the problem worse. Hence a step wise treatment regime is instituted until success is met or patient fatigue sets in!
Usually starting from simple things (steroid / silicone gel) and getting more interventional – ultimately intra-lesional excision coupled with post-op radiotherapy
While a scar cannot be removed they can often be significantly improved
- Making a wide scar narrower
- Reorientating/repositioning a scar (To be more aesthetically aligned with other structures)
If due to a registered ACC injury then ACC will often cover the full cost of scar revision.